Stroke survivors trial new at-home tech: 'It's given me my freedom back'
Source: BBC Technology
Stroke Survivors Trial New At‑Home Tech: “It’s Given Me My Freedom Back”
19 hours ago
Shiona McCallum – Senior technology reporter

BBC
Amanda James‑Hammett was just 37 when she had a stroke while doing the dishes at home.
“I heard a pop in my head, like a big bubble. I tried to scream, but it wasn’t a normal scream. I knew something wasn’t right.”
Within hours, Amanda lost the ability to speak and move her right arm. She later had to relearn how to talk, read and carry out everyday tasks.
Six years on, she has taken part in a nationwide NHS trial testing a new at‑home device that could help stroke survivors regain hand and arm movement.
“It’s about freedom. It’s given me my freedom back.” – Amanda
The Trial
- Name: Triceps trial
- Funding: £2 million
- Scope: 19 NHS sites across the UK, led by Sheffield Teaching Hospitals NHS Foundation Trust in partnership with the University of Sheffield
- Goal: Recruit ~270 participants; the largest brain‑stimulation‑for‑stroke trial ever conducted
“Stroke is an interruption to the blood supply to the brain,” says Dr Sheharyar Baig, neurologist at Sheffield’s Royal Hallamshire Hospital. “When the blood supply is interrupted, the brain stops functioning in that area, leading to weakness, visual problems, speech problems, and more.”
Common Stroke Signs
- Facial weakness – difficulty smiling; one side of the face may droop
- Arm weakness – inability to fully lift or hold up an arm due to weakness or numbness
- Speech problems – slurred words or confused speech
If you notice any of these symptoms, call 999 immediately.
Why This Matters
- Stroke is the leading cause of adult‑onset disability in the UK, affecting about 100,000 people a year.
- Over one million people live with its long‑term effects.
- Roughly half of stroke survivors experience ongoing arm weakness, ranging from reduced dexterity to complete loss of movement.
- Arm weakness hampers everyday tasks such as dressing, cooking, and working, adding pressure to health and social‑care services.
Shifting recovery from hospital to the home environment could be vital for improving outcomes and easing the burden on the NHS. The Triceps trial aims to do just that by testing technology that empowers survivors to regain independence.
How the device works
Participants in the Triceps trial use a small electrical device that sits inside the ear and stimulates the vagus nerve—a major nerve connecting the brain and abdomen—while carrying out rehabilitation exercises.

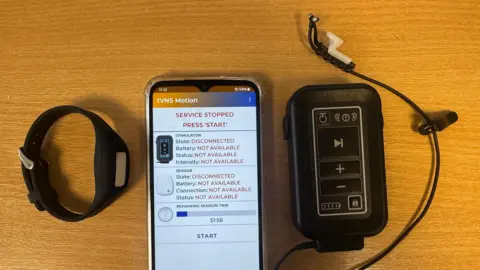
“The recovery process is unfortunately quite slow for many people,” says Dr Baig, adding that it can involve lots of effort and hours of rehabilitation.
“So we’re interested in ways we can boost the effects of rehab and create a brain environment that’s more responsive to it.”
Unlike earlier versions of vagus‑nerve stimulation, which required surgery to implant a device, this treatment is non‑invasive and can be used at home. Dr Baig notes that the pulses sent by the ear‑piece are set at a level that is comfortable and painless.
“A New Woman”
Amanda used the device for up to an hour a day as part of her rehab over 12 weeks, combining it with exercises and everyday tasks.
“At first I didn’t think it was going to work at all,” she says.
“But after a couple of weeks, I started to see changes in my hand.”
One of the biggest milestones for her was returning to sewing – a passion she could not initially pursue after her stroke.

Amanda is back in the sewing room.
Amanda says she feels like “a new woman” now that she can cut material and use her sewing machine again.
“I can put my socks on, I can do my shoes, I can do my house,” she tells the BBC.
“I don’t have to wait for anyone else.”
Early Improvements
So far, more than 200 people have taken part in the trial. While researchers do not yet know who is receiving active stimulation and who is receiving placebo, they say early signs are promising.
“We have seen some wonderful improvements in people’s arm function,” Dr Baig says.
He also stresses the treatment is not a cure, but something that could help people in everyday life.
“Someone who was unable to carry a cup of tea with one arm can now walk from room to room holding it stably,” he explains.
“Another participant set their post‑stroke personal best in a 5 km run and noticed their arm function was better while running.”
The results of the Triceps trial are being closely monitored by the Stroke Association, which is part‑funding the research.
“The team are doing brain imaging and taking blood tests because we know that some stroke patients really respond well to this technology while some don’t,” said Maeva May, the charity’s Associate Director of Systems Engagement.
“We want to understand which patients respond best and how.”
Dr Baig adds that, if effective, the technology could be quite scalable because it is affordable, convenient, and can be easily integrated into existing rehab services.
For Amanda, the impact is already clear:
“It’s about being independent again. Those small things make a big difference.”
Images

